Typically, there is a prolonged period—averaging more than seven years—between the initial infection with HIV and the onset of AIDS, during which patients may remain entirely asymptomatic.
According to international research and extensive clinical experience, the majority of patients with AIDS present with oral symptoms one to four years prior to the actual onset of the disease. These symptoms manifest as various oral lesions and serve as crucial indicators for the detection and diagnosis of HIV infection.
By possessing the following knowledge, dental practitioners can potentially identify and diagnose infected individuals and patients, thereby enabling the implementation of necessary therapeutic measures. This not only serves to save patients' lives but also helps mitigate the risks of occupational exposure that may arise during subsequent dental treatments.
I. Classification of Oral Lesions Associated with AIDS Based on Severity
In 1992, based on the oral manifestations of AIDS, the World Health Organization (WHO) established a set of classification and diagnostic criteria, categorizing oral lesions associated with AIDS into the following three groups based on their severity:
Group 1: Oral lesions strongly associated with HIV infection. This category comprises five specific conditions: oral candidiasis, oral hairy leukoplakia, HIV-associated periodontal disease, Kaposi's sarcoma, and non-Hodgkin lymphoma.
Group 2: Oral lesions associated with HIV infection. This category includes non-specific oral ulceration, salivary gland disease, thrombocytopenic purpura, and various viral infections.
Group 3: Oral manifestations that may be seen in the context of HIV infection. Examples include bacterial infections, epithelioid angiomatosis, adverse drug reactions, cryptococcosis, and histoplasmosis.
The oral manifestations of AIDS constitute one of the key indicators for diagnosing the disease; indeed, the majority of individuals infected with HIV exhibit some form of oral manifestation. Consequently, these signs must be given serious attention.
Oral Candidiasis
This condition is further subdivided into two types: the erythematous type and the pseudomembranous type. Lesions frequently occur on the attached gingiva and oral mucosa, which serve as specific sites of predilection; white spots or patches may occasionally be observed within the erythematous (reddened) areas of the lesion. However, lesions may also develop in any part of the oral cavity, presenting as white or yellow spots or patches. These patches are typically friable—meaning they can be wiped away—leaving behind an erythematous underlying surface that may bleed.
Numerous epidemiological studies have demonstrated that oral candidiasis exhibits a remarkably high prevalence among HIV-infected populations. It can occur at various stages of HIV infection, with prevalence rates reaching as high as 96%. Oral candidiasis is frequently the initial manifestation of HIV infection and constitutes the most common type of oral lesion; in the vast majority of cases, it serves as an early sign of post-HIV immunosuppression, indicating the potential emergence of other opportunistic infections.
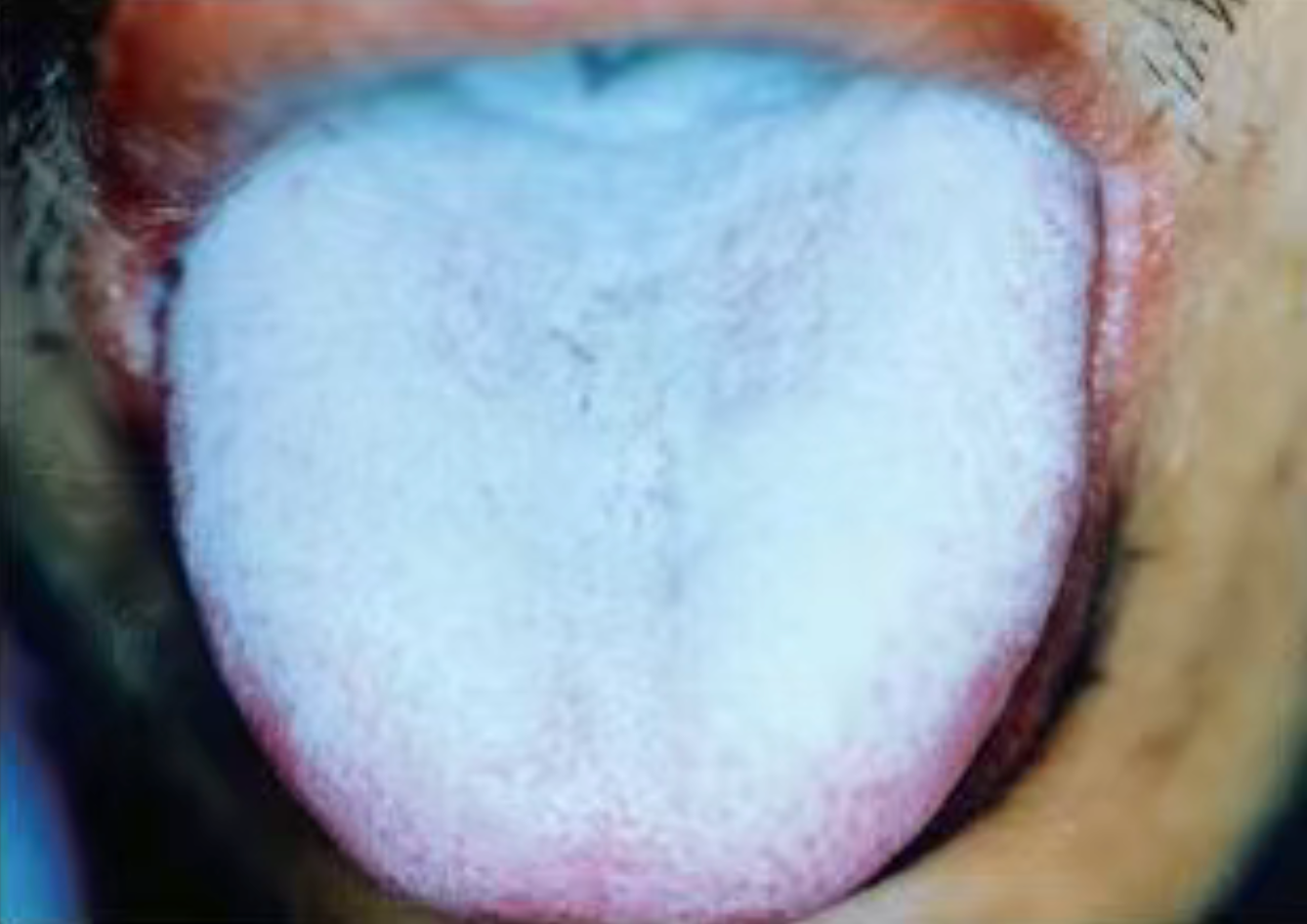
*Candida albicans* Infection Model
Oral Hairy Leukoplakia
Some researchers suggest that oral candidiasis and oral hairy leukoplakia may serve as indicators for detecting or predicting HIV infection.
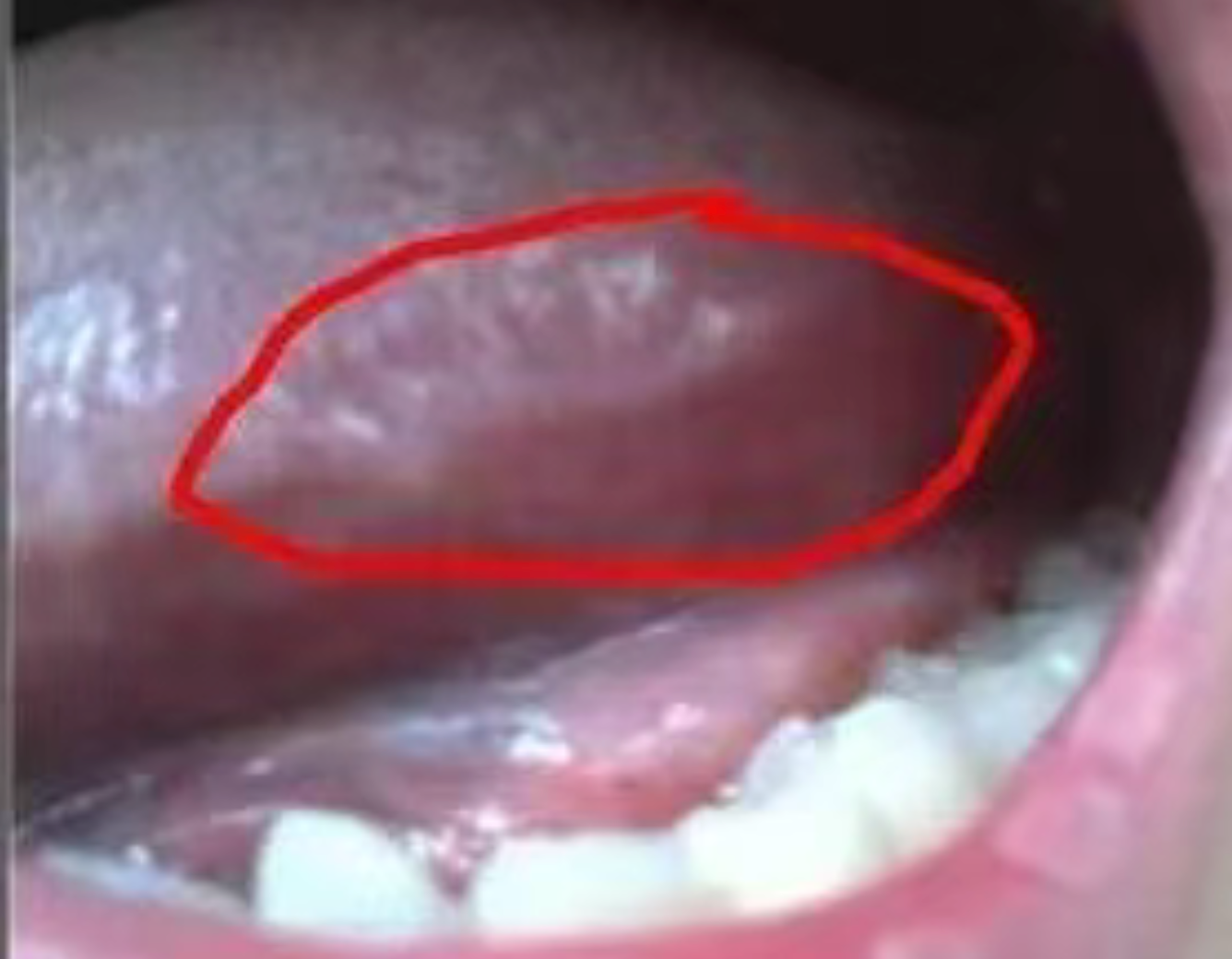
Oral hairy leukoplakia presents as white or gray lesions occurring along the lateral margins of the tongue; these lesions may also extend to the ventral and dorsal surfaces of the tongue and cannot be wiped away. Among individuals with HIV infection or AIDS, oral hairy leukoplakia is the second most common oral manifestation—surpassed only by candidiasis—and serves as a hallmark of HIV-related disease. It is observed almost exclusively within the HIV-infected and AIDS patient populations, demonstrating a remarkably high degree of specificity.
Consequently, the appearance of oral hairy leukoplakia warrants close attention. Periodontal disease manifests as gingival inflammation, ulceration, and necrosis, as well as tooth mobility; associated symptoms may include gingival bleeding, pain, and—in rare instances—malignant transformation.
Kaposi's Sarcoma
Kaposi's sarcoma has become a common malignancy among individuals infected with HIV. The tumor may develop on the skin or the oral mucosa. Within the oral cavity, the palate is the most frequently affected site, followed by the gingiva. The tumors typically present as deep red or purplish-red nodules or plaques that do not blanch upon digital pressure; surrounding ecchymoses (bruising) of a yellowish-brown hue may also be present.
Kaposi's sarcoma is rare in the general population; however, with the AIDS epidemic, it has emerged in significant numbers among populations at risk for AIDS. In the United States, the likelihood of an AIDS patient developing Kaposi's sarcoma is at least 20,000 times greater than that of the general population.
Among the oral manifestations observed in individuals infected with HIV and patients with AIDS, Kaposi's sarcoma ranks second only to candidiasis and oral hairy leukoplakia in terms of prevalence, exhibiting a relatively high incidence rate.
Periodontal Diseases, Oral Mucosal Diseases, etc.
Periodontal diseases manifest as gingival inflammation, ulceration, and necrosis, as well as tooth loosening; symptoms such as gingival bleeding, pain, and malignant transformation may also occur. It has been reported that 19% to 29% of individuals infected with HIV or suffering from AIDS present with periodontitis.
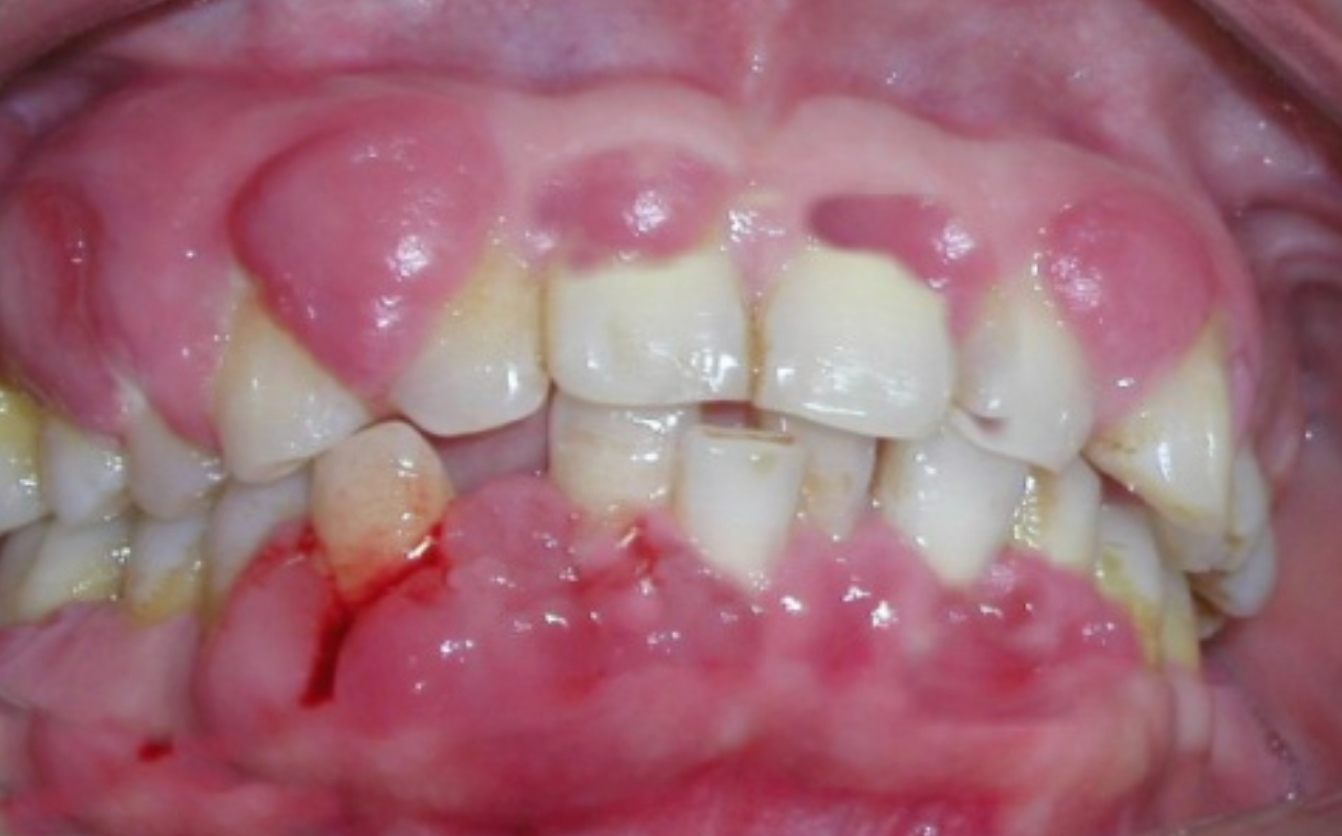
Let us look specifically at oral ulcers. They are classified into two types:
The first type is recurrent aphthous stomatitis, which may manifest as solitary or clustered lesions; it can also develop into major aphthous ulcers—large, deep lesions accompanied by severe pain.
The second type consists of nonspecific ulcers; these are characterized by a prolonged course, mild pain, and a fixed location—most commonly on the palate. They tend to be chronic and slow to heal, and are often surrounded by a distinct white halo (indicative of a *Candida albicans* infection).
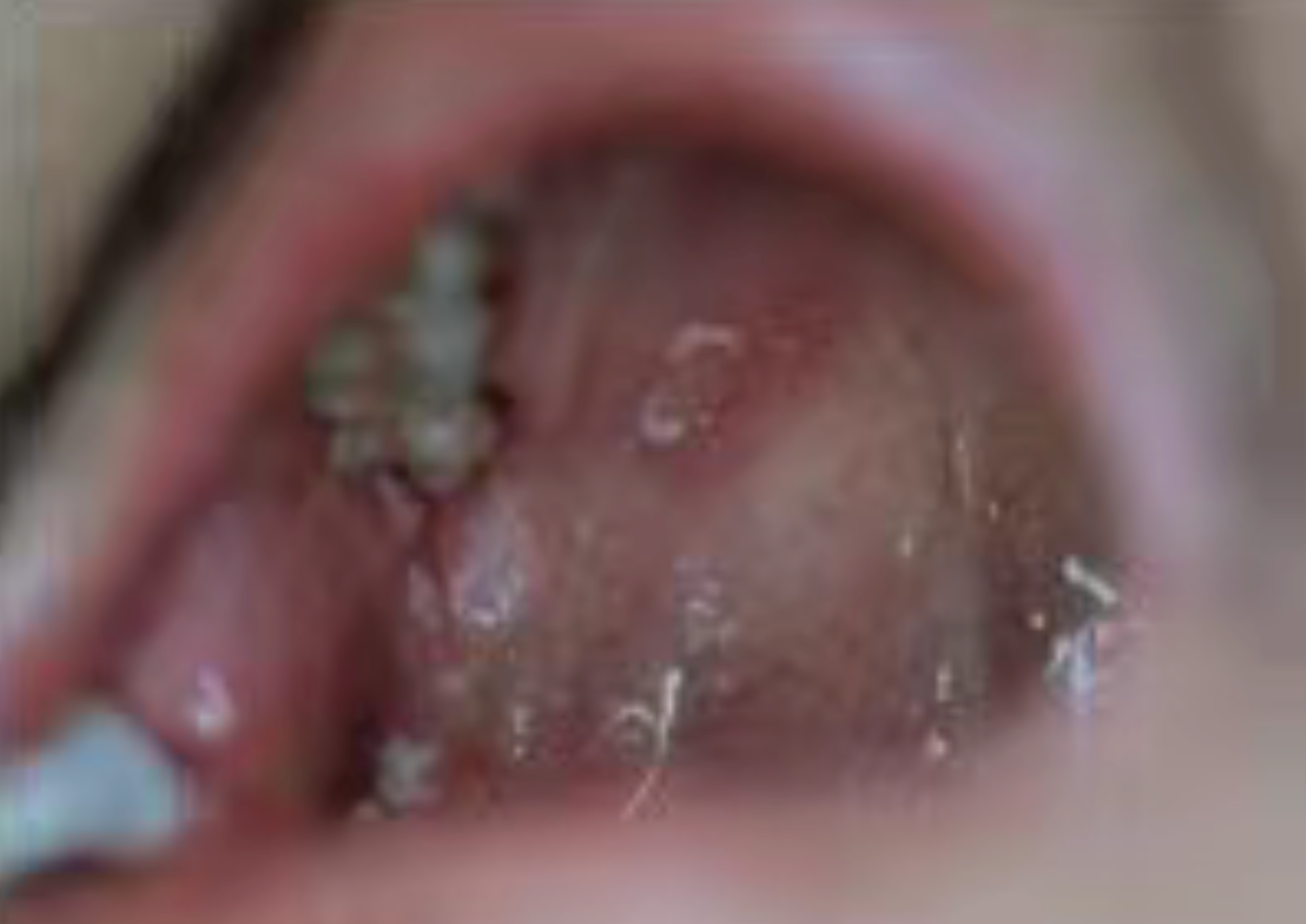
II. Occupational Exposure Prevention for Dentists—Consider HIV Post-Exposure Prophylaxis
Given the persistently high prevalence of HIV/AIDS today, dental practitioners face a constant occupational risk due to their frequent exposure to patients' blood and saliva. Furthermore, since many oral diseases serve as key indicators for the early diagnosis of HIV/AIDS, it is imperative that dentists prioritize their own personal protection while providing patient care.
Here, we focus specifically on HIV post-exposure prophylaxis (PEP). We urge all dentists to commit the following information to memory—though we sincerely hope you will never actually need to use it!
HIV post-exposure prophylaxis—commonly referred to by its English acronym, PEP—typically refers to a regimen of medications taken following a high-risk exposure event to prevent the HIV virus from establishing an infection. PEP does not consist of a single drug, but rather a combination of several medications. These regimens are available in two forms: dual-drug combinations and triple-drug combinations. The dual-drug regimen consists of two antiviral medications and is relatively more affordable; however, the triple-drug regimen is significantly more effective!
High-risk exposure events include unprotected sexual contact with an individual with HIV/AIDS; contact between open wounds or mucous membranes and the blood of an individual with HIV/AIDS; and accidental puncture injuries caused by needles or sharp instruments contaminated with the blood of an individual with HIV/AIDS.
Besides, dentists should use the high quality of disposable medical gloves to protect themselves.
